It's 1:47 a.m. You're sitting in front of the bathroom mirror, or curled on the couch with your phone face-down, and you've just done it again. You promised yourself this morning you wouldn't. You meant it. There's a small mark on your jaw, or a scab on your shoulder you've reopened for the fourth time this week, and now you're searching to find out why your brain keeps doing this when you've explicitly told it not to.
You're not weak. You're not gross. You're not the only one. There is a real, specific reason your brain keeps pulling you back to your skin even when every conscious part of you wants to stop. This article is about that reason.
We'll keep it honest. No clinical coldness, no toxic positivity, no twelve-step plan dressed up as an answer. Just the actual science of what's happening, why willpower keeps losing the race, and what that means for what you can do next.
Key takeaways
- Skin picking that you can't stop is a recognized condition called dermatillomania (excoriation disorder), classified in the DSM-5 since 2013.
- It affects roughly 3.4% of the general population — about one in twenty-nine people. Most have never told a doctor.
- The behavior taps into your brain's reward circuitry. Picking gives a brief, real shift — relief, focus, or a sense of completion — and your brain learns to seek it.
- Once the loop is established, the basal ganglia (habit center) takes over from your prefrontal cortex (decision-making). "Deciding to stop" doesn't work the same way as deciding what to eat for breakfast.
- The shame–picking–shame cycle makes it worse. Shame raises stress, and stress is one of the most common triggers.
- Recovery is possible. Habit Reversal Training (HRT) is the gold-standard behavioral treatment. It works by interrupting the loop, not by trying harder.
The short answer
You can't stop because your brain has learned that picking solves something for it, even though it costs you everything else. Every time you pick, your brain registers a small shift — researchers describe it as activity in reward circuitry that gets reinforced, not necessarily a clean dopamine spike (Grant et al., 2022). The picking briefly down-regulates anxiety, briefly satisfies a sensory urge, briefly delivers a sense of completion. Your conscious mind hates the result. Your reward system doesn't care.
Once that loop runs enough times, the behavior gets handed off from the part of your brain that makes decisions to the part that runs habits. At that point, "just stop" becomes roughly as effective as telling yourself to stop blinking. You can do it for a while if you concentrate. The moment your attention drifts, the system that was running in the background takes over again.
The willpower failure isn't a character flaw. It's the predictable outcome of a brain doing exactly what brains are designed to do: repeating behaviors that produced relief in the past.
It's a recognized condition with a name
The behavior you're describing has a clinical name: excoriation disorder, also called dermatillomania or skin-picking disorder. It's one of the body-focused repetitive behaviors (BFRBs), alongside trichotillomania (hair pulling) and several others. Here's a deeper look at what dermatillomania is.
If you've never seen the term before, you're in the majority. Most primary care providers still aren't trained to recognize it, and most people who pick their skin spend years assuming it's just a bad habit they should be able to fix.
It's also far more common than you'd guess.
That puts dermatillomania at a higher prevalence than OCD, body dysmorphic disorder, and several other conditions you've probably heard far more about. It's not rare. It's just under-discussed, partly because of the visible scarring, and partly because the shame around it keeps people from saying the words out loud.
A separate study of 10,169 adults representative of the U.S. population found that 2.1% met criteria for current skin-picking disorder, and 3.1% had a lifetime history (Grant & Chamberlain, 2020). Most of them had never told a doctor. In a separate Grant lab sample of 262 adults with skin-picking disorder, 87% had never received any treatment for it (Grant et al., 2022). That gap says far more about under-recognition in primary care than about anyone's motivation.
The neurology in plain English
Here's what's happening inside your head when you pick.
Your brain has two systems that compete for control of your behavior. The first is the prefrontal cortex, the slow, deliberate, decision-making part. It's the part of you reading this article and saying "right, I see, I need to stop." The second is the basal ganglia, the fast, automatic, habit-running part. It's the part of you that drives home from work without remembering the route. It runs sequences of behavior in the background, frees up your attention for other things, and is built to be efficient, not thoughtful.
Picking gets handed off from the first system to the second.
The first few times you pick, it's a deliberate act. There's a bump, a scab, a sensation, and your prefrontal cortex makes a (somewhat) conscious choice to address it. But picking, for reasons we'll get to in a second, produces a small reward signal in your brain. Neuroimaging studies in BFRBs have documented altered reward-circuit activity and impulse-control patterns (Roberts et al., 2018; reward-circuitry findings reviewed in Grant et al., 2022). Your reward system flags the behavior as worth repeating.
After enough repetitions, the basal ganglia takes the wheel. The behavior runs as a habit, triggered by cues you may not even notice consciously: a moment of boredom, a specific seat on the couch, a particular emotion, even just the texture of a scab against your fingertip.
This is the key thing. Once a behavior is running on the basal ganglia, your prefrontal cortex isn't really driving anymore. You can override the habit if you catch it early and apply concentrated attention. But "deciding to stop" only works in the narrow window before the habit fires, and the habit fires faster than conscious thought.
That's why willpower keeps losing the race. It's not that your willpower is weak. It's that you're trying to win a sprint with a system that's structurally slower.

There's a second piece. The behavior doesn't just become automatic. It becomes functional. Picking is doing a job for your brain. For different people, that job is different:
- Soothing. Picking down-regulates anxiety. The repetitive motion plus the small sensory hits act like a self-administered calming protocol. Anxiety goes down for a few minutes after a session.
- Stimulating. When you're under-stimulated (bored, working on something tedious, watching TV), picking gives the brain a reliable, predictable source of input. Many people pick most when they're bored, not when they're stressed.
- Completing. There's a felt sense that the bump is "wrong" and removing it will make things "right." Pursuing that resolution recruits the same circuitry as any other goal-directed behavior. The fact that it never actually works (there's always another bump) doesn't matter to the loop.
- Sensory. For many people, especially those with sensory processing differences, the texture of skin and the precise feel of picking is its own draw. The behavior provides a specific sensation the brain seeks out.
None of those needs vanish when you decide to stop. Which leads to the next part.
Why you pick even though you want to stop
This is the part that hurts. You know it's hurting you. You've sworn off it dozens of times. You feel awful afterward. And you do it anyway.
Two things are happening.
The first is the wanting-to-stop paradox. Your conscious decision to stop lives in the prefrontal cortex. The picking lives downstream of reward signaling and habit circuitry. These two systems run on different timescales and respond to different inputs. Your prefrontal cortex can't directly override the habit any more than it can directly tell your heart rate to slow down. It can influence the habit indirectly, over time, with the right kind of practice. But it can't just decide its way out.
The second is the shame loop. You pick. You feel awful. The shame and self-criticism spike your stress. Stress is one of the most reliable triggers for picking. In Grant and Chamberlain's 2022 sample of 262 adults with skin-picking disorder, stress and the texture of the skin were the two most commonly reported triggers. So the shame you feel about the last episode increases the probability of the next one.
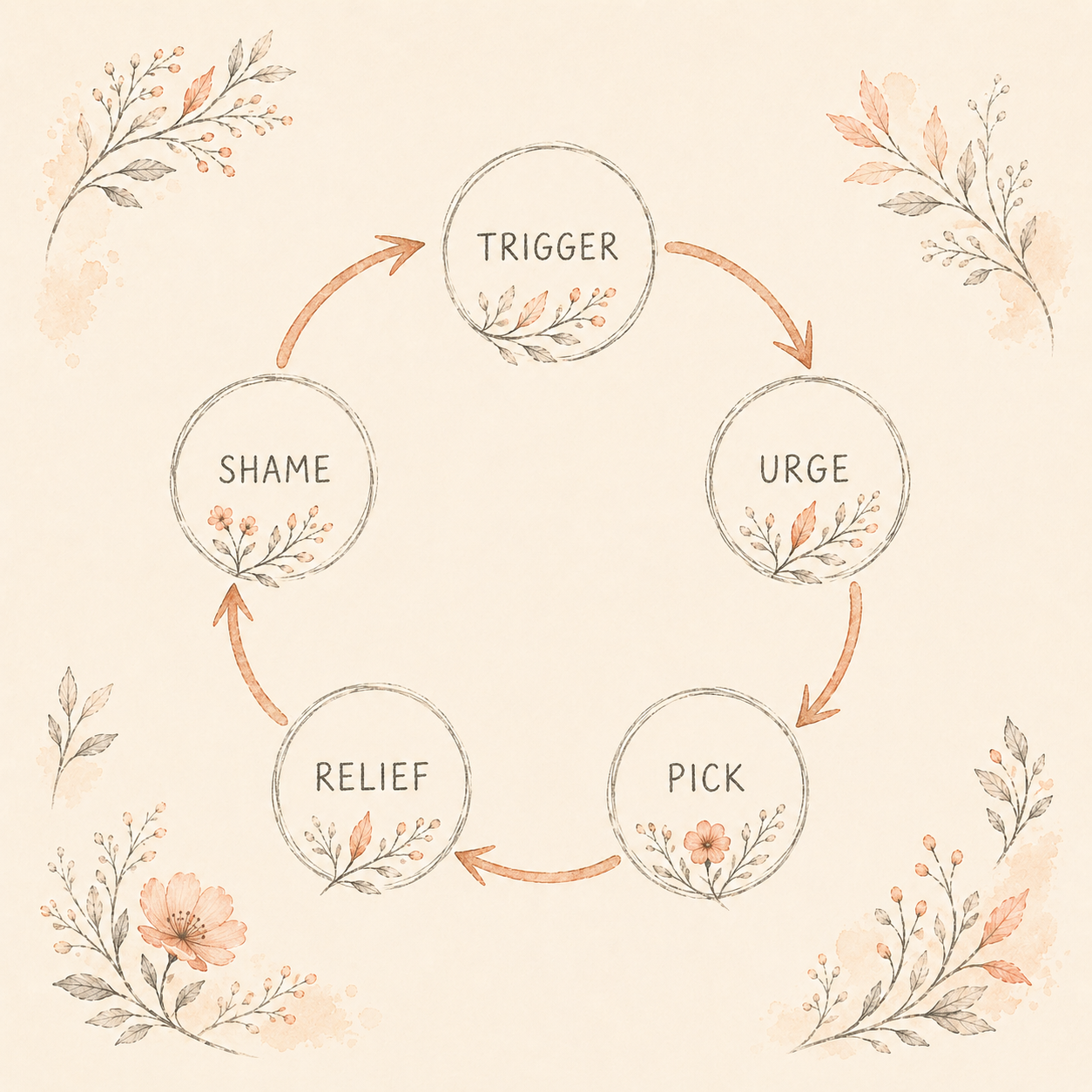
Naming this loop is most of the relief. The shame isn't a sign that you're a bad person who needs to feel worse. The shame is a symptom of the same circuitry, and treating it as more evidence against yourself only feeds the cycle.
If you take one thing from this article: when you pick, the most useful response is not self-criticism. It's noticing, with as little drama as possible, what just happened, and getting back to whatever you were doing. The neurological reason for that recommendation isn't "be nice to yourself." It's that compassion lowers stress, and lower stress means fewer triggers.
The role of ADHD, anxiety, OCD, and autism
If you suspect you have ADHD, anxiety, OCD, or autism (or you're already diagnosed with one of them) and you also pick, you are very much not imagining a connection. The overlap is real, and it's significant.
Source: Grant & Chamberlain, 2020 — community survey of 10,169 U.S. adults. Specialist-clinic samples often show higher rates, particularly for ADHD and autism in youth populations (Rautio et al., 2024).
The reason these conditions cluster together isn't mysterious. They share underlying themes. ADHD brains are often under-stimulated and seek input; picking provides reliable, predictable sensory input. Anxious brains run hot; picking down-regulates that arousal. OCD brains get stuck on perceived imperfections; the bump on your face is a perceived imperfection your brain won't release. Autistic brains often have sensory regulation needs that picking, like other stimming behaviors, can meet.
This means picking isn't just a "bad habit" you developed for no reason. For many people, it's a strategy that emerged to solve a real problem the brain was having. The strategy is harmful, but the underlying need is legitimate. There's a longer piece here on the ADHD–dermatillomania overlap specifically.
This framing matters because it changes the goal. The goal isn't to stop picking by sheer force and leave the underlying need unmet. The goal is to find ways to meet the need that don't damage your skin. Habit Reversal Training is built around exactly that principle.
What this means for stopping
You can stop. The path looks nothing like white-knuckled willpower.
Habit Reversal Training (HRT) is the leading evidence-based treatment for BFRBs, including skin-picking disorder (Lee et al., 2019). It works by giving you tools to do three things: notice the urge before the picking starts, identify what need the picking is meeting in that moment, and substitute a behavior that meets the need without the cost. Done consistently, HRT produces meaningful reductions in picking severity in published trials.
The reason it works isn't magic. It works because it operates on the actual mechanism: it builds awareness in the narrow window between urge and action where the prefrontal cortex still has a vote, and it trains a competing response that the basal ganglia can eventually adopt as the new default.
If you want a tactical guide, we have one: how to stop skin picking — a practical guide based on HRT principles. This article isn't that. This article was about answering your actual question, which was why.
If understanding the why was useful and you want a tool that puts these mechanisms to work day-to-day (logging episodes and urges, tracking your patterns, working through HRT modules at your own pace), that's exactly what SkinAware was built for.
Ready to Start Tracking?
SkinAware helps you log episodes, identify patterns, and see real progress over time.
FAQ
The short version: not by trying harder. The behavior runs on automatic circuits that conscious effort can't directly override. The evidence-based approach is Habit Reversal Training, which works by building awareness of the urge before picking starts and substituting a competing response. Most people see meaningful improvement over weeks to months of consistent practice, not days.
Yes, when it's chronic, distressing, and you've repeatedly tried to stop. The clinical name is excoriation disorder (also called dermatillomania), and it's been a recognized DSM-5 diagnosis since 2013. Occasional picking at a hangnail isn't the disorder. The diagnosis applies when the behavior causes tissue damage, distress, or impairment, and you've tried unsuccessfully to reduce or stop it.
Neither, technically. It's its own condition, classified alongside OCD in the same DSM-5 category but distinct from both. That said, the overlap is large: roughly a quarter of people with skin-picking disorder also have ADHD, and a similar proportion have OCD in community samples (Grant & Chamberlain, 2020). Specialist clinic samples often show much higher rates, particularly for ADHD in youth (up to 41%, Rautio et al., 2024). If you have one, screening for the others is worth doing.
It can resemble both, and for some people it functions partly as both. Stimming refers to self-stimulatory behavior that regulates sensory input or arousal, common in autism and ADHD. Some skin picking is functionally stimming. It can also resemble compulsions in OCD, where the picking is driven by an intrusive sense that something is wrong and must be fixed. The clinical category for skin-picking disorder sits adjacent to OCD specifically because of these compulsive features, but the dominant function varies person to person.
Because the behavior isn't really about the bumps. It's about the loop the bumps trigger. Once the loop is established, your brain will find something to pick: a tiny pore, a healing scab, even smooth skin that "feels" off. This is one of the strongest signs that the behavior is functioning as a self-regulation strategy rather than a response to actual skin imperfections.
Yes. Recovery isn't always linear, and "stopping" usually looks more like meaningful reduction with occasional lapses than perfect cessation overnight. The evidence is genuinely encouraging: HRT-based treatment produces meaningful reductions in picking severity, and NHS guidance recommends CBT that includes habit reversal for excoriation disorder. The barrier for most people isn't that recovery doesn't work. It's that they never knew there was a name for what they have, or where to start.
The short version: not by trying harder. The behavior runs on automatic circuits that conscious effort can't directly override. The evidence-based approach is Habit Reversal Training, which works by building awareness of the urge before picking starts and substituting a competing response. Most people see meaningful improvement over weeks to months of consistent practice, not days.
Yes, when it's chronic, distressing, and you've repeatedly tried to stop. The clinical name is excoriation disorder (also called dermatillomania), and it's been a recognized DSM-5 diagnosis since 2013. Occasional picking at a hangnail isn't the disorder. The diagnosis applies when the behavior causes tissue damage, distress, or impairment, and you've tried unsuccessfully to reduce or stop it.
Neither, technically. It's its own condition, classified alongside OCD in the same DSM-5 category but distinct from both. That said, the overlap is large: roughly a quarter of people with skin-picking disorder also have ADHD, and a similar proportion have OCD in community samples (Grant & Chamberlain, 2020). Specialist clinic samples often show much higher rates, particularly for ADHD in youth (up to 41%, Rautio et al., 2024). If you have one, screening for the others is worth doing.
It can resemble both, and for some people it functions partly as both. Stimming refers to self-stimulatory behavior that regulates sensory input or arousal, common in autism and ADHD. Some skin picking is functionally stimming. It can also resemble compulsions in OCD, where the picking is driven by an intrusive sense that something is wrong and must be fixed. The clinical category for skin-picking disorder sits adjacent to OCD specifically because of these compulsive features, but the dominant function varies person to person.
Because the behavior isn't really about the bumps. It's about the loop the bumps trigger. Once the loop is established, your brain will find something to pick: a tiny pore, a healing scab, even smooth skin that "feels" off. This is one of the strongest signs that the behavior is functioning as a self-regulation strategy rather than a response to actual skin imperfections.
Yes. Recovery isn't always linear, and "stopping" usually looks more like meaningful reduction with occasional lapses than perfect cessation overnight. The evidence is genuinely encouraging: HRT-based treatment produces meaningful reductions in picking severity, and NHS guidance recommends CBT that includes habit reversal for excoriation disorder. The barrier for most people isn't that recovery doesn't work. It's that they never knew there was a name for what they have, or where to start.
Continue Reading
References
- American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
- Farhat, L. C., Lin, A., Flores, J. M., et al. (2023). Prevalence and gender distribution of excoriation (skin-picking) disorder: A systematic review and meta-analysis. Journal of Psychiatric Research, 162, 34–41.
- Grant, J. E., & Chamberlain, S. R. (2020). Prevalence of skin picking (excoriation) disorder. Journal of Psychiatric Research, 130, 57–60.
- Grant, J. E., Dougherty, D. D., & Chamberlain, S. R. (2022). Characteristics of 262 adults with skin picking disorder. Comprehensive Psychiatry, 117, 152338.
- Lee, M. T., Mpavaenda, D. N., & Fineberg, N. A. (2019). Habit Reversal Therapy in Obsessive Compulsive Related Disorders: A Systematic Review. Frontiers in Behavioral Neuroscience, 13, 79.
- Rautio, D., et al. (2024). Body-focused repetitive behaviors in a specialist youth clinic. (Comorbidity data on ADHD/autism.)
- Roberts, S., O'Connor, K., & Bélanger, C. (2018). Emotion regulation and other psychological models for body-focused repetitive behaviors. Clinical Psychology Review, 31(5), 745–762.
